
A linear ablation set was completed, anchored to electrically inert regions. The flutters terminated with radiofrequency ablation at the area of slow conduction between the superior vena cava (SVC) and the tricuspid annulus (TA). Ablation was performed at 25–50 W for 10–30 seconds per lesion. In the latter, the flutter was initially assessed to be CTI-dependent, but CTI ablation caused a change in flutter cycle length without termination ( Figure 2), leading to remapping and diagnosis of macroreentrant flutter dependent on slow conduction through scar on the superior RA. In 7 of 8 cases, a CTI ablation had been performed either in a prior procedure (3 cases) or during the present procedure (4 cases). Local activation was timed relative to a stable coronary sinus reference. Catheter mapping and ablation were performed using the Biosense Webster (Irvine, CA) CARTO 3-dimensional electroanatomical mapping system and an irrigated, force-sensing catheter. 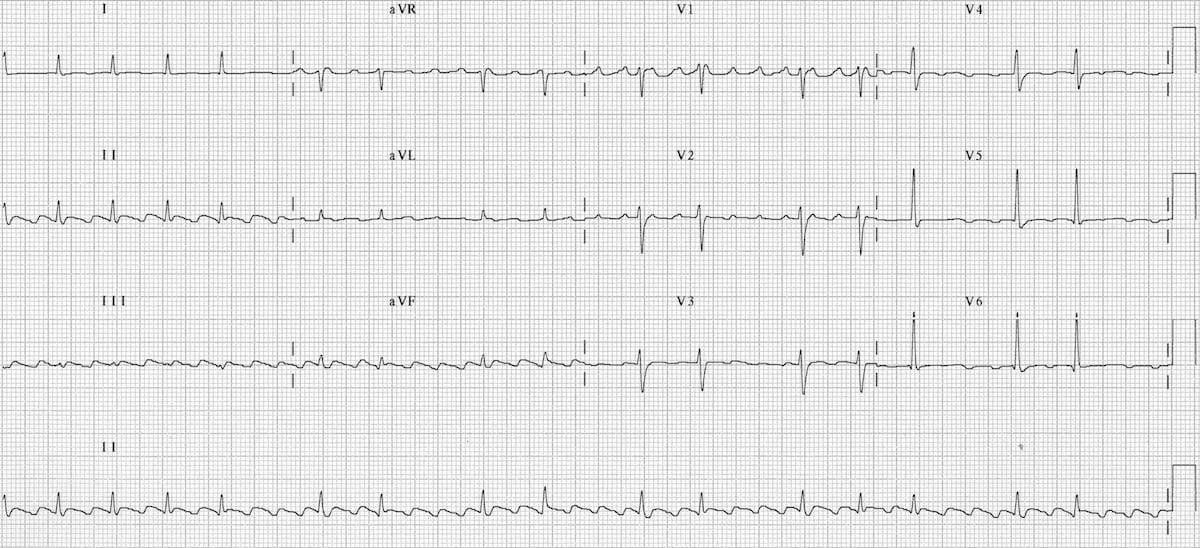 
Some patients presented in atrial flutter and in other cases, arrhythmias were induced with atrial pacing. The surface electrocardiogram P-wave morphology and tachycardia cycle length (260-490 ms) of the flutter were variable. Patient ages ranged from 55 to 78 years and pre-ablation left ventricular ejection fraction from 35% to 65%. An electrophysiology (EP) study and ablation were performed from 1 month to 14 years after surgery. The original operative report was not available for 1 case. One patient also had a tricuspid valve repair through the same right atriotomy incision. Original operative reports were available in 7 of the patients, and all these patients had a superior septal approach to the mitral valve for acquired valve disease. We report the mapping and ablation of 8 patients with macroreentrant atrial flutters that were dependent on slow conduction through an area of scar on the superior RA in the setting of prior surgical mitral valve repair or replacement. In contrast to atriotomy flutter following a lateral RA incision, macroreentry RA flutter from a superior septal incision is less well-described in the literature. Then, the surgeon incises the fossa ovalis and extends this to join the RA incision at the superior septum, where the incision is continued into the dome of the left atrium to expose the mitral valve ( Supplemental Figure 1). 7, 8 The surgeon makes a vertical incision in the RA starting near the atrioventricular groove and carried cephalad around or through the RA appendage to the superior portion of the atrial septum. 1, 4, 5, 6 An alternate approach to the mitral valve, the superior septal approach, provides excellent exposure of the mitral valve for repair or replacement. 1, 2, 3 Atriotomy flutter involving a lateral RA incision, often coexistent with cavotricuspid isthmus (CTI)-dependent flutter, is well described. Macroreentrant right atrial (RA) tachycardias have been reported following surgical incision of the atrium to treat acquired and congenital heart disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
